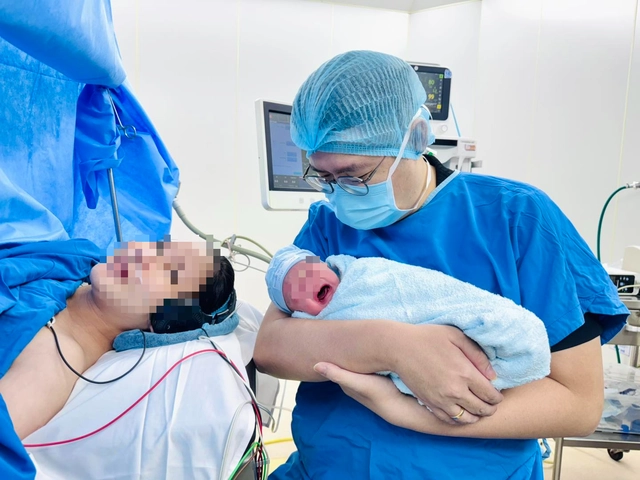
A medical staff holds a 3.2-kilogram baby boy who was safely delivered at Tu Du Hospital in Ho Chi Minh City on February 25, 2026, nearly two months after doctors performed a 30-minute fetal cardiac intervention. Photo: Supplied
The hospital said the child was delivered by cesarean section at 39 weeks of pregnancy earlier that day.
His heart and breathing were stable at birth, and he quickly adapted to life outside the womb.
The successful delivery marked the end of a high-risk pregnancy for his 27-year-old mother, identified as N.T.T., a city resident.
She was the 12th patient to undergo a successful fetal cardiac intervention at Tu Du Hospital in coordination with Children's Hospital 1, with the procedure performed on December 30, 2025.
It was her second pregnancy and was conceived naturally, and it had initially progressed without complications.
First-trimester ultrasound scans found no abnormalities, while non-invasive prenatal testing indicated a low risk of genetic disorders.
However, between 22 and 24 weeks of gestation, a detailed fetal echocardiogram detected structural heart abnormalities, including severe pulmonary valve stenosis accompanied by tricuspid regurgitation.
She was then referred to the two hospitals for consultation and close monitoring.
Amniocentesis later confirmed a normal chromosomal profile, an important finding that enabled doctors to consider in-utero intervention to improve the baby's prognosis.
Follow-up assessments showed the fetal heart disease progressing, with increasing underdevelopment of the right ventricle.
Without intervention, doctors warned the fetus was at risk of progressing to single-ventricle physiology, a complex congenital heart defect that typically requires multiple staged surgeries after birth and carries a poor prognosis.
Following an inter-hospital consultation, doctors agreed to perform a fetal cardiac catheterization to dilate the pulmonary valve under ultrasound guidance.
The aim was not only to address the valve stenosis at the time of intervention but also to restore blood flow through the pulmonary valve, maintain right ventricular development, and preserve the possibility of achieving a two-ventricle — or at least one-and-a-half-ventricle — circulation after birth.
At 10:00 am on December 30, 2025, when the fetus was 29 weeks old, a joint medical team from the two hospitals successfully performed the fetal cardiac catheterization.

N.T.T., 27, and her husband share a joyful moment after the successful fetal cardiac intervention performed on December 30, 2025 at Tu Du Hospital in Ho Chi Minh City. Photo: Xuan Mai / Tuoi Tre
This was the first fetal cardiac catheterization carried out after the Ministry of Health approved the official technical list for the specialty, marking an important step forward in mastering advanced fetal medicine techniques in Vietnam.
The mother was closely monitored after the procedure.
Subsequent ultrasounds showed improved blood flow and continued development of the right ventricle, suggesting a favorable response.
Dr. Tran Ngoc Hai, director of Tu Du Hospital, said the most striking aspect of the case was the procedure's duration.
The entire operation was completed in under 30 minutes, a sharp reduction from earlier cases that had taken several hours, including one that required two attempts totaling six hours.
"By the 12th case, our team had gained substantial experience and was able to finish the procedure in less than half an hour," Hai said, adding that the shorter operating time reflected growing technical mastery and confidence.
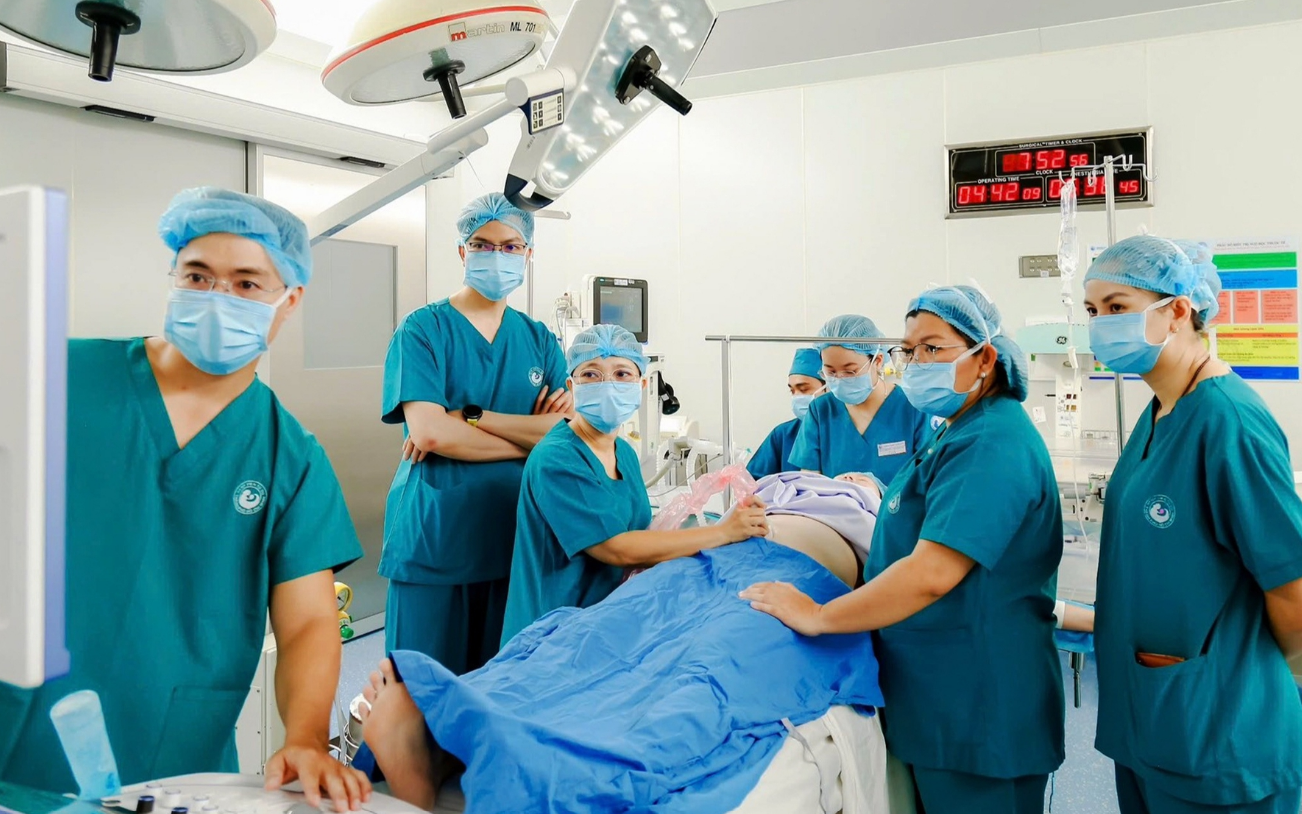
Fetal cardiac intervention is an advanced, highly specialized procedure that requires close coordination among obstetrics, pediatric cardiology, anesthesiology and resuscitation, and diagnostic imaging.
Doctors said the successful birth not only brought relief to one family but also highlighted the steadily advancing capabilities of Vietnamese medical centers in mastering sophisticated techniques and managing risks in fetal care.


Max: 1500 characters
There are no comments yet. Be the first to comment.